HOME / NEWS / Industry News / How to Swab for Flu: Step-by-Step Guide and Swab Types Explained
What Does a Flu Swab Actually Do?
A flu swab collects a sample of mucus and cellular material from the nasal passage or throat, where influenza viruses concentrate during active infection. The swab is then tested—either through a rapid antigen test or a more sensitive PCR assay—to detect the presence of influenza A or B viral proteins.
The quality of the swab itself directly affects test accuracy. A swab that releases collected material efficiently and does not absorb or retain the sample in its fibers produces more reliable results. This is why clinical-grade swabs made from polyester or microfiber materials have largely replaced cotton in diagnostic settings—they release up to 90% of collected sample volume compared to roughly 50–60% for traditional cotton fiber swabs.
How to Swab for Flu: Step-by-Step
Whether you are performing a flu swab in a clinical setting or using an at-home rapid test kit, the technique follows the same essential steps. Incorrect swabbing is one of the leading causes of false-negative results in influenza testing.
- Wash hands thoroughly before handling the swab or test components to avoid contaminating the sample.
- Remove the swab from packaging without touching the tip. Hold the swab only by the handle.
- Tilt your head back slightly and insert the swab tip into one nostril. For a nasopharyngeal swab, gently advance the swab along the floor of the nasal cavity until slight resistance is felt—approximately 2–3 inches in adults. For an anterior nasal swab (used in most at-home kits), insert only about 0.5–1 inch.
- Rotate the swab 3–5 times against the mucosal surface, maintaining gentle pressure for 5–10 seconds to ensure adequate sample collection.
- Repeat in the second nostril using the same swab (for most at-home tests) or a fresh swab if clinically indicated.
- Transfer the swab into the extraction tube or transport medium immediately, following the kit manufacturer's instructions for agitation and immersion time.
- Apply the extracted fluid to the test strip and wait for the indicated result window—typically 10–15 minutes for rapid antigen tests.
For throat swabs used in some rapid tests, firmly swab the tonsillar area and posterior pharynx, avoiding the tongue and inner cheeks, which reduces viral yield.
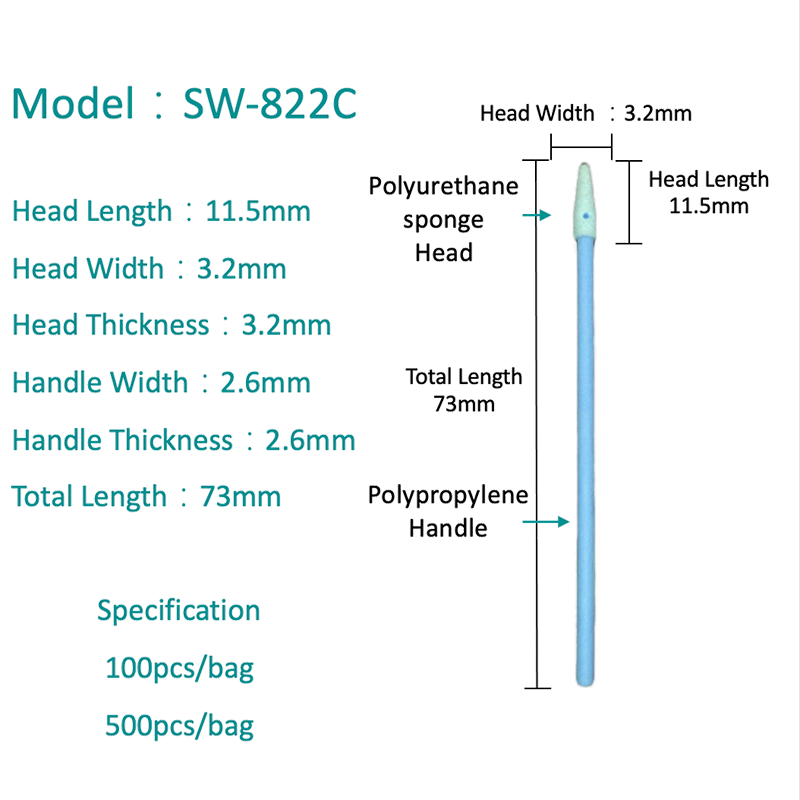
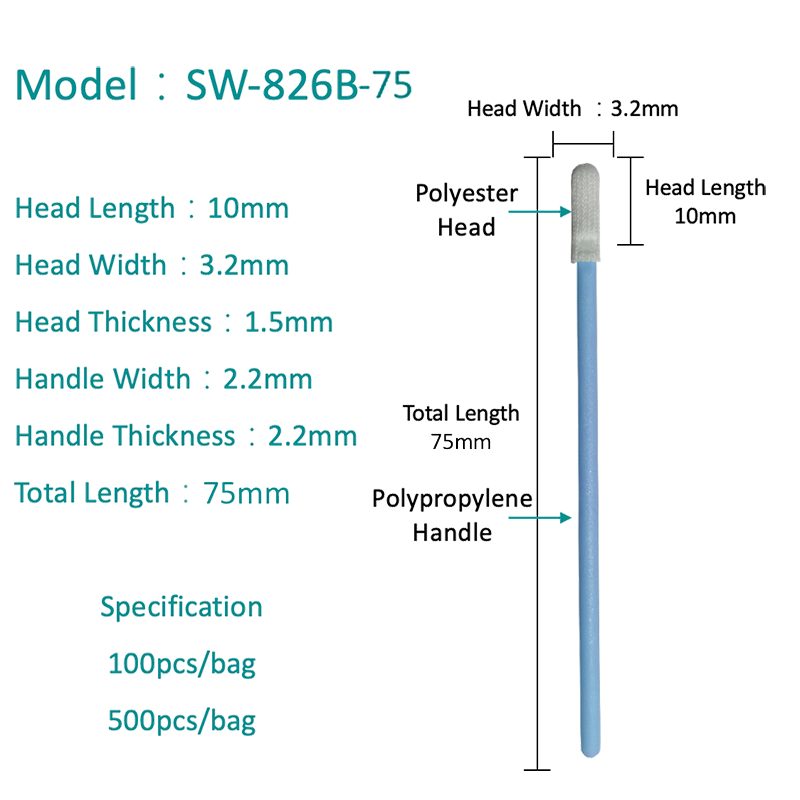
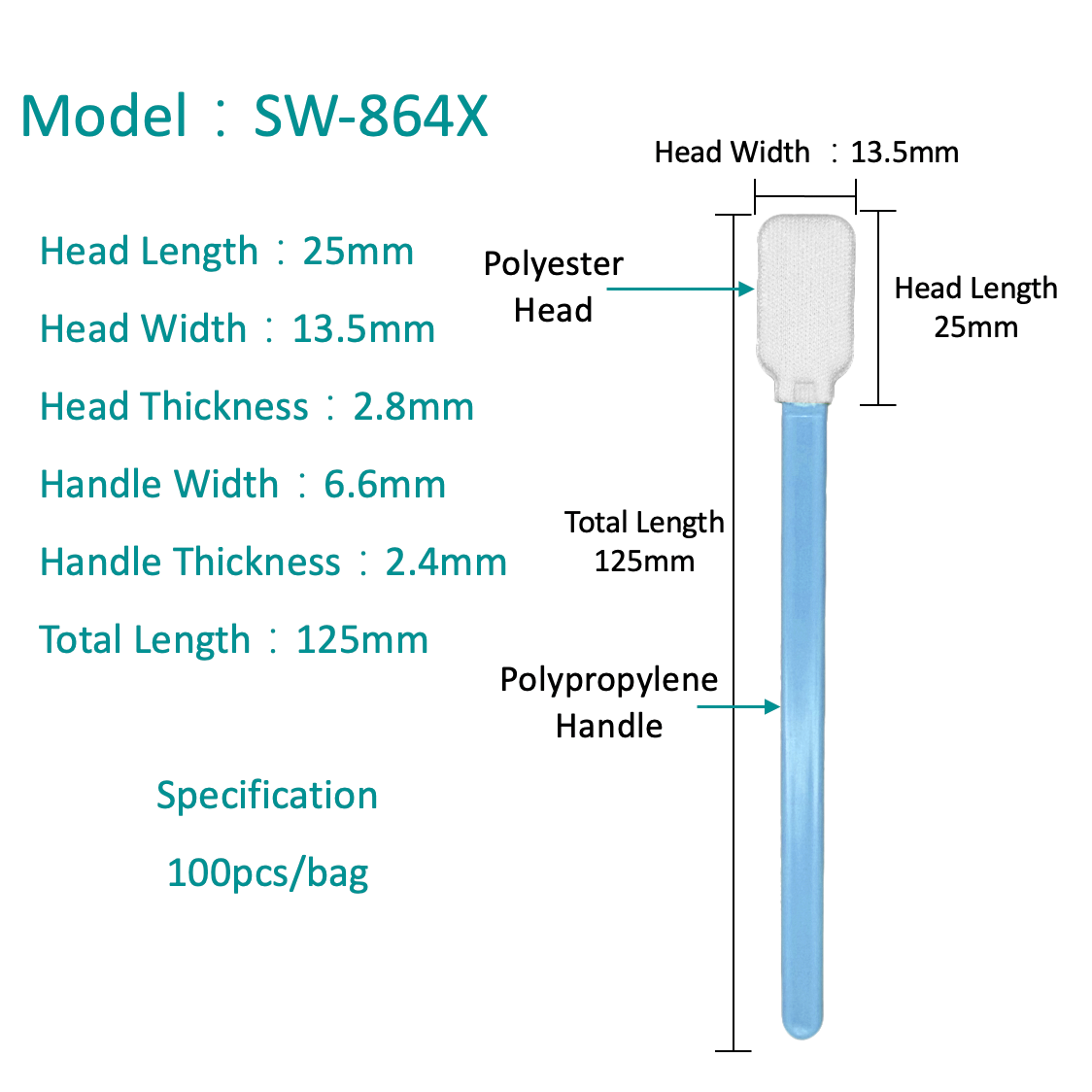
Types of Flu Swabs: Choosing the Right Material
Not all swabs perform equally in viral diagnostics. The fiber material, tip construction, and shaft flexibility all influence how much virus is captured and how efficiently it is eluted into test reagents.
| Swab Type | Material | Sample Release Rate | Typical Application |
|---|---|---|---|
| Cotton Swab | Natural cotton fiber | ~50–60% | General sampling (legacy use) |
| Polyester Swab | Synthetic polyester fiber | ~85–92% | Viral diagnostics, PCR, rapid tests |
| Microfiber Cleanroom Polyester Swab | Ultra-fine polyester microfiber | >90% | High-sensitivity PCR, cleanroom, IVD |
| Flocked Swab | Nylon flocked tip | >90% | Nasopharyngeal sampling, influenza |
Why Polyester and Microfiber Outperform Cotton
Polyester swabs are non-absorbent by nature—their synthetic fibers do not wick fluid inward the way cotton does, so the collected viral material remains at the surface of the tip where it can be transferred into extraction reagent efficiently. This property is critical in flu testing, where viral load can be low, particularly early in infection or in vaccinated individuals with partial immunity.
Microfiber cleanroom polyester swabs take this further. The ultra-fine fiber construction creates a high surface area that captures more particles per unit contact, while the cleanroom manufacturing environment ensures the swab is free of particulates, endotoxins, and nucleases that could degrade RNA samples and interfere with PCR amplification. These swabs are particularly important for real-time RT-PCR flu testing, where even minor RNA degradation reduces assay sensitivity.
Common Mistakes That Lead to False-Negative Flu Results
Specimen collection errors account for a significant share of inaccurate flu test results. Studies evaluating influenza rapid antigen tests have reported false-negative rates ranging from 20% to 50% depending on test kit and collection technique. The following errors are the most frequently documented:
- Insufficient insertion depth — Only inserting the swab 1–2 cm captures primarily anterior nasal cells and mucus, missing the higher-yield nasopharyngeal region where influenza virus replicates most actively.
- Too little rotation time — A single pass without dwelling on the mucosal surface collects a fraction of the available viral material. Rotating for at least 5 seconds significantly improves yield.
- Using the wrong swab type — Some test kits specify a particular swab material. Substituting cotton for polyester can inhibit the PCR reaction due to cotton's natural tannins and inhibitory compounds.
- Testing too early or too late — Viral shedding peaks in the first 24–72 hours of symptom onset. Testing after day 5 of illness often yields lower viral loads that fall below rapid test detection thresholds.
- Improper swab storage — Leaving a collected swab unrefrigerated for more than 4 hours before transfer to transport medium degrades RNA and reduces test sensitivity.
Selecting Flu Swabs for Clinical and Point-of-Care Settings
For clinical laboratories and point-of-care facilities procuring swabs for influenza testing programs, several specifications should be evaluated beyond fiber material alone:
- Shaft flexibility and breakpoint — Nasopharyngeal swabs require a flexible shaft that can navigate the nasal anatomy without patient discomfort. Swabs with a designated breakpoint allow the tip to be deposited directly into transport tubes.
- Sterility certification — For clinical diagnostics, individually sterile-packaged swabs are standard. Cleanroom polyester swabs manufactured under ISO Class 5 or better conditions reduce the risk of nucleic acid contamination in molecular workflows.
- Compatibility with transport media — Confirm that the swab material is validated for use with the viral transport medium (VTM) or universal transport medium (UTM) in your workflow. Some fiber materials interact with certain preservatives and reduce viral viability.
- DNA/RNA-free certification — For PCR-based flu testing, swabs should be certified free of exogenous nucleic acids to prevent false amplification signals.
Microfiber cleanroom polyester swabs meet the most demanding specifications across all of these categories, making them the preferred choice for high-throughput molecular diagnostic laboratories and hospital infection control programs where test accuracy directly informs treatment and isolation decisions.




 English
English  中文简体
中文简体