HOME / NEWS / Industry News / How to Do Strep, Flu & Nasal Swabs: Types, Techniques & Testing Guide
What Are Cotton Swabs Made For — Medical vs. Diagnostic vs. Consumer Use
The term "swab" covers a wide range of collection and application tools, and the substrate material, tip geometry, and shaft composition are all intentionally engineered for specific tasks. Using the wrong swab type is one of the most common sources of false-negative results in rapid diagnostic testing.
Standard household cotton swabs — the kind sold in drugstores for cosmetic and household use — are made with cotton fiber wound or bonded onto a paper or plastic shaft. They are designed for surface application, makeup removal, and cleaning small areas. They are explicitly not suitable for diagnostic specimen collection because:
- Cotton fibers can inhibit PCR amplification by releasing compounds that interfere with polymerase enzyme activity.
- Cotton tips retain specimen material rather than releasing it efficiently into transport media.
- Shaft dimensions are not standardized to fit collection tubes or transport vials.
Diagnostic-grade swabs used in medical settings are engineered differently. The most common types include:
- Flocked swabs — nylon fibers applied perpendicularly to the shaft tip via electrostatic flocking. This creates a brush-like surface with dramatically improved cell collection and elution efficiency compared to wound-fiber tips. The standard choice for respiratory virus PCR testing.
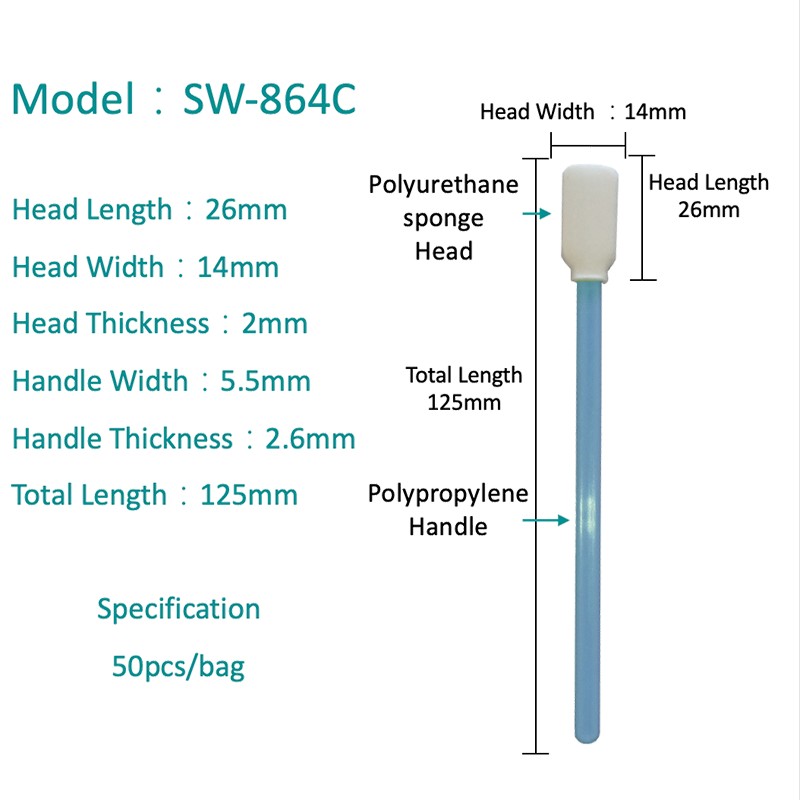
- Foam swabs — open-cell polyurethane foam tips absorb and release liquid specimens efficiently. Used in wound cultures and some antigen rapid tests.
- Rayon/dacron swabs — synthetic fiber tips that are PCR-compatible and used widely in throat and nasopharyngeal collection; less efficient than flocked swabs but lower cost.
- Calcium alginate swabs — used historically for gonorrhea and chlamydia cultures; largely superseded by synthetic alternatives as alginate can inhibit certain molecular assays.
Long Q-tip swabs in clinical contexts refers to extended-shaft swabs — typically 15–20 cm in length with a flexible wire or thin plastic shaft — used specifically for nasopharyngeal (NP) collection, where the swab must travel the full length of the nasal passage to reach the posterior nasopharynx. Standard 7–10 cm throat swabs cannot reach this anatomy.

How to Do a Strep Swab: Technique, Anatomy, and Common Errors
A throat swab for Group A Streptococcus (GAS) — the bacterium responsible for strep throat — is the most commonly performed diagnostic swab in primary care settings. The sensitivity of rapid strep antigen tests ranges from 70–90% and PCR-based throat swabs from 95–99%, but both are highly dependent on correct collection technique. A poorly performed swab can easily produce a false-negative even when the patient is genuinely infected.
Preparation
- Use a sterile rayon, dacron, or flocked throat swab — not cotton.
- Have the patient seated upright with head tilted slightly back and mouth fully open.
- Use a light source (penlight or otoscope) to visualize the posterior oropharynx.
- Depress the tongue gently with a tongue depressor to prevent contamination of the swab tip with saliva or tongue flora.
Collection Technique
- Identify the target zones: the posterior pharyngeal wall and both tonsillar pillars (or tonsillar fossae if tonsils have been removed). These are the primary sites of GAS colonization — not the soft palate, uvula, or tongue.
- Swab the posterior pharyngeal wall and both tonsillar areas with firm, rolling pressure. Apply enough contact pressure to collect epithelial cells and exudate, not just surface moisture.
- Rotate the swab while moving it across the surfaces — a single drag without rotation collects significantly fewer cells.
- Complete the collection in 3–5 seconds. Prolonged contact increases gag reflex activation and patient movement, which reduces specimen quality.
- Do not touch the teeth, tongue, cheeks, or lips with the swab tip — oral flora contamination reduces assay specificity and can produce invalid rapid test results.
After Collection
For rapid antigen detection tests (RADT), insert the swab immediately into the extraction reagent tube per manufacturer protocol. For culture or PCR send-out, place the swab in the appropriate transport medium (Amies or Stuart for culture; universal viral/bacterial transport medium for PCR) and label with collection time. GAS is sensitive to desiccation — specimens for culture should reach the laboratory within 24 hours, or within 72 hours if held in transport medium at 2–8°C.
How to Perform a Flu Swab: Nasal, Nasopharyngeal, and Combined Approaches
Influenza testing is performed using rapid influenza diagnostic tests (RIDTs), immunofluorescence assays, or molecular PCR panels. The swab collection site significantly affects test sensitivity — nasopharyngeal swabs consistently outperform anterior nasal swabs for influenza detection, particularly later in the illness course when viral shedding in the anterior nasal passage declines but remains elevated in the posterior nasopharynx.
Anterior Nasal Swab for Flu (Self-Collection / Rapid Test)
Many FDA-cleared home flu tests and point-of-care RIDTs are designed for anterior nasal collection, which is easier to perform without clinical training:
- Insert the swab tip approximately 2–2.5 cm (about one inch) into one nostril — just past the nasal vestibule.
- Rotate the swab in a full circle against the nasal wall 5 times, applying gentle but consistent pressure.
- Withdraw and repeat the same motion in the other nostril using the same swab — bilateral collection significantly increases cell yield and sensitivity.
- Process immediately per the test kit instructions. Anterior nasal specimens are particularly time-sensitive for RIDTs.
Nasopharyngeal Swab for Flu (Clinical Setting)
NP swab collection for influenza follows the same anatomical approach described below for COVID-19 NP collection. The key difference is swab selection: flu NP swabs must be compatible with the downstream assay — most molecular flu panels specify flocked NP swabs in universal transport medium (UTM). Do not use calcium alginate swabs for influenza PCR, as alginate inhibits reverse transcriptase enzymes used in flu RT-PCR assays.
PCR Nasal Swab vs. Nasopharyngeal Swab for COVID-19: Differences That Matter
During the COVID-19 pandemic, the comparison between anterior nasal (AN) swabs and nasopharyngeal (NP) swabs for SARS-CoV-2 PCR testing became clinically significant. Both collection methods are valid, but they differ in sensitivity, patient comfort, training requirements, and appropriate use context.
| Feature | Anterior Nasal (AN) Swab | Nasopharyngeal (NP) Swab |
|---|---|---|
| Insertion depth | ~2 cm into nostril | Full nasal passage length (~8–10 cm) |
| Swab type | Short rigid or semi-flexible flocked | Long flexible flocked (wire or thin plastic shaft) |
| Relative sensitivity (PCR) | ~85–92% vs. NP reference | Reference standard (~95–98%) |
| Patient discomfort | Minimal | Significant — tearing, gagging common |
| Trained collector required | No — self-collection validated | Yes — clinical training required |
| Best use case | Symptomatic early-stage testing, screening | High-stakes clinical decisions, late-stage illness |
Nasopharyngeal Swab Collection Procedure
NP swab collection requires specific technique to reach the correct anatomical target — the mucosa overlying the posterior nasopharynx — and to avoid the most common collection errors:
- Position the patient seated upright with head tilted back approximately 70° — this aligns the nasal floor with the nasopharynx and reduces resistance during insertion.
- Select the clearer nostril. If the patient reports nasal congestion or septal deviation, use the more patent side. Do not attempt to force the swab through an obstructed passage.
- Insert the swab horizontally — parallel to the hard palate, not angled upward toward the nasal bridge. Angling upward is the most frequent technique error; it causes pain, epistaxis, and collects turbinate cells rather than nasopharyngeal cells.
- Advance slowly until resistance is felt at the posterior wall — typically at a depth equal to the distance from the nostril to the tragus of the ear (approximately 8–10 cm in adults).
- Dwell and rotate: hold the swab at the posterior wall for 5–10 seconds, rotating gently to collect columnar epithelial cells. Do not force or scrape aggressively.
- Withdraw slowly while continuing to rotate. Place immediately into the transport medium tube and break the shaft at the scored line.
Mid-turbinate (MT) swabs represent a practical middle ground — inserted 2–3 cm deeper than AN but not to the full NP depth. Studies have found MT collection sensitivity for SARS-CoV-2 PCR to be 90–95% of NP sensitivity, with substantially better patient tolerability. Many clinical guidelines now accept MT swabs as the preferred alternative to full NP collection in outpatient and community testing settings.
Cheek Swab Genetic Testing: Collection, Accuracy, and Applications
Buccal (cheek) swabs are the standard non-invasive collection method for DNA-based genetic testing. The buccal mucosa sheds epithelial cells continuously, and these cells carry the full nuclear genome — identical in DNA sequence to cells collected from blood, saliva, or any other tissue. Cheek swab DNA yield is typically 1–10 µg per swab, sufficient for most genotyping arrays, ancestry analysis panels, and paternity testing without amplification.
How to Collect a Buccal Swab
- Do not eat, drink, smoke, or chew gum for at least 30 minutes before collection — food particles, beverages, and saliva dilute the epithelial cell concentration on the swab and can introduce PCR inhibitors.
- Open the swab packaging without touching the tip.
- Place the swab tip against the inner cheek wall (buccal mucosa), not the tongue or gum.
- Rub the swab tip firmly back and forth along the cheek wall 10–15 times, rotating while rubbing to collect cells from all swab surfaces.
- Allow the swab to air-dry for 30–60 seconds before placing it in the provided envelope or container — wet swabs sealed immediately can develop mold during shipping, which degrades DNA.
- If the kit includes multiple swabs (common for paternity and forensic testing), repeat for each swab on the same cheek or alternate cheeks per instructions.
Applications of Cheek Swab Genetic Testing
- Ancestry and direct-to-consumer genomics — services such as 23andMe and AncestryDNA use buccal swabs to genotype 600,000–700,000 SNPs (single nucleotide polymorphisms) across the genome, enabling ancestry composition estimates and relative matching.
- Paternity and relationship testing — STR (short tandem repeat) profiling from buccal cells achieves the same statistical confidence as blood-based DNA testing. Accredited laboratories report paternity probabilities exceeding 99.99% from a single buccal collection.
- Pharmacogenomics — cheek swabs are used by clinical and direct-to-consumer PGx panels (e.g., GeneSight, Genomind) to identify variants in CYP450 enzyme genes affecting drug metabolism. Results inform prescribing decisions for antidepressants, antipsychotics, and anticoagulants.
- Newborn and pediatric screening — buccal swabs provide a painless alternative to heel-prick blood collection for certain neonatal genetic screening programs.
- Bone marrow donor registries — organizations such as DKMS and Be The Match use buccal swabs to HLA-type potential donors for their registries, enabling matching with patients requiring stem cell transplantation.
One important limitation of buccal swab DNA: it cannot detect somatic mutations present only in tumor or blood cells. For cancer genetic testing that requires analysis of circulating tumor DNA or hematologic malignancy variants, blood-based liquid biopsy or tissue biopsy samples are required. Buccal swabs reflect germline (inherited) DNA only.




 English
English  中文简体
中文简体